Can Cell Therapy Restore Hearing Loss?
Post by Anastasia Sares
The takeaway
In an experimental cell therapy treatment, researchers transplanted young, immature auditory cells from the ears of newborn mice into older mice whose hearing had been damaged. These cells, surrounded by a new environment, matured and repaired the hearing of the older mice.
What's the science?
Deep in the inner ear are cells called hair cells that are responsible for taking sound from the environment and turning it into electrical signals to be sent to the brain. These cells are attached to a membrane in the ear that vibrates with incoming sounds, and the movement of this membrane causes the cells to fire. However, as we age, hair cells experience significant wear and tear, and they are sensitive to insults like loud noise exposure, infections, and head trauma. There are even certain classes of drugs that can cause hair cells to die off as a side effect. Hair cells generally do not regenerate in adults, so when they die, it causes an irreversible loss in hearing. While there are some solutions for hair cell loss, such as cochlear implants, these all come with their own drawbacks.
Cell therapy is a kind of medical treatment that involves taking cells from one organism and transplanting them into another (or from one organ/tissue to another within the same organism). It includes treatments like bone marrow transplants and stem cell therapy. When trying to apply this kind of therapy to hearing loss, there are several challenges: will the transplanted cells develop into functioning hair cells? Will the procedure be too invasive and cause additional damage to the inner ear? Will the procedure result in significantly better hearing in the end?
This week in Neuroscience, Liu and colleagues showed that cells can be successfully transplanted into the inner ear and restore hearing function in mice that have drug-induced hearing loss.
How did they do it?
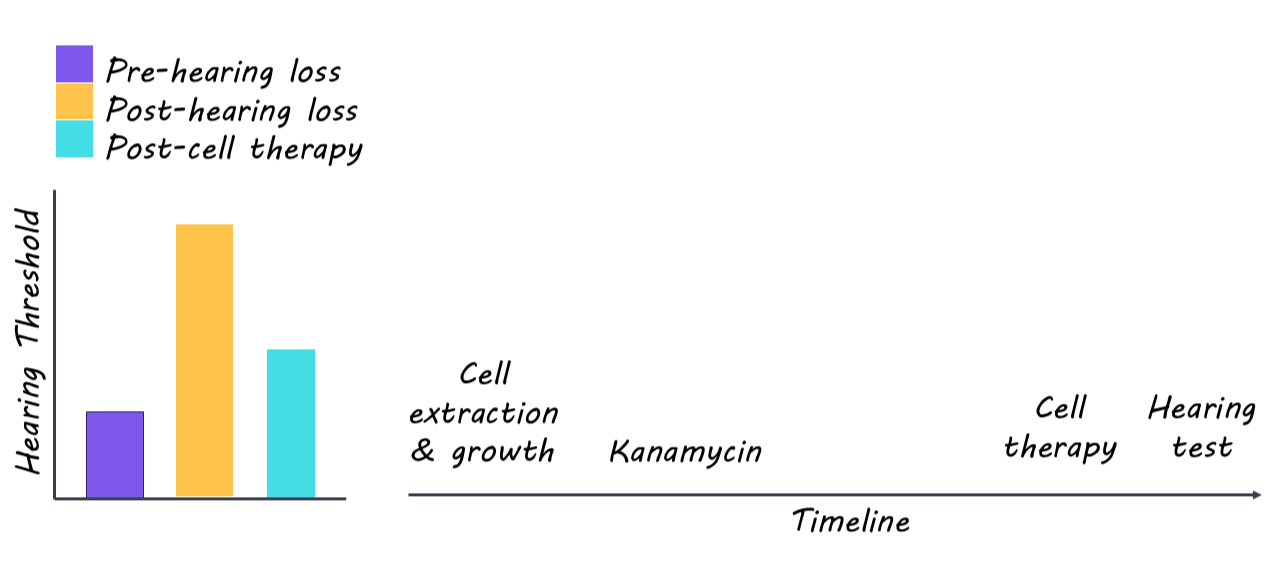
The authors first induced hearing loss in a group of adult mice by administering an antibiotic known to cause hair cell death (kanamycin). Then, relying on previous research, they extracted a very specific type of cell from the inner ears of newborn mice and grew these cells in a gel matrix, where the cells clumped together to form small “organoids” that were ready to become hair cells. They then injected these cells into the left inner ear of each adult mouse (with the right ear serving as a control).
To measure the mice’s hearing, the authors used the auditory brainstem response, which records electrical activity from the brainstem to measure how well the early auditory system responds to sound. They made these measurements before hearing loss, after hearing loss, and after cell therapy.
What did they find?
The authors confirmed that hair cells had died and that the adult mice’s hearing was severely impaired after being exposed to kanamycin. After cell therapy, hair cells survived the transplant and did not cause any additional hearing loss in the mice. The new cells were able to repopulate the inner ear, and hearing thresholds recovered substantially (though not completely) following the cell therapy.
What's the impact?
This study shows that it is possible to restore the function of hair cells and significantly improve hearing using cell therapy. Cell therapy may be a viable way to address the previously irreversible problem of hearing loss that affects millions of people worldwide.