Using Brain Lesions to Identify a Common Addiction Brain Circuit
Post by Megan McCullough
The takeaway
Brain lesions brought on by brain damage from events such as strokes have been known to interrupt addiction in some individuals with substance use disorders and even lead to remission. Lesion mapping shows that these regions connect to a specific brain circuit that can be used as a therapeutic target for the treatment of addiction.
What's the science?
Substance use disorders (SUDs) are a leading cause of death in young populations. Neuromodulation of brain regions implicated in addiction — a current therapy for addiction — involves delivering electrical stimuli to induce changes in specific neural circuits. However, there is a need to better identify therapeutic targets for neuromodulation. Previous research has shown that brain damage from strokes has led to addiction remission in some individuals with SUD. This week in Nature Medicine, Joutsa and colleagues aimed to link brain lesions that resulted in addiction remission to the human connectome in order to gain a better understanding of the specific brain regions involved in addiction remission.
How did they do it?
The authors examined data from 129 patients who were daily nicotine smokers at the time they acquired a brain lesion, with a subset of these patients entering addiction remission right after the lesion. Lesion locations within the patients entering addiction remission were analyzed to identify the specific brain regions connected with remission. The authors next tested if lesions within the addiction remission cohort mapped to a specific brain circuit rather than a single brain region. Utilizing lesion network mapping, connectivity patterns between lesion locations were then compared across groups: those entering remission versus non-quitters. Finally, the authors looked at which brain voxels [a location in three-dimensional space] have a similar connectivity profile to the profiles of the lesion locations that led to addiction disruption.
What did they find?
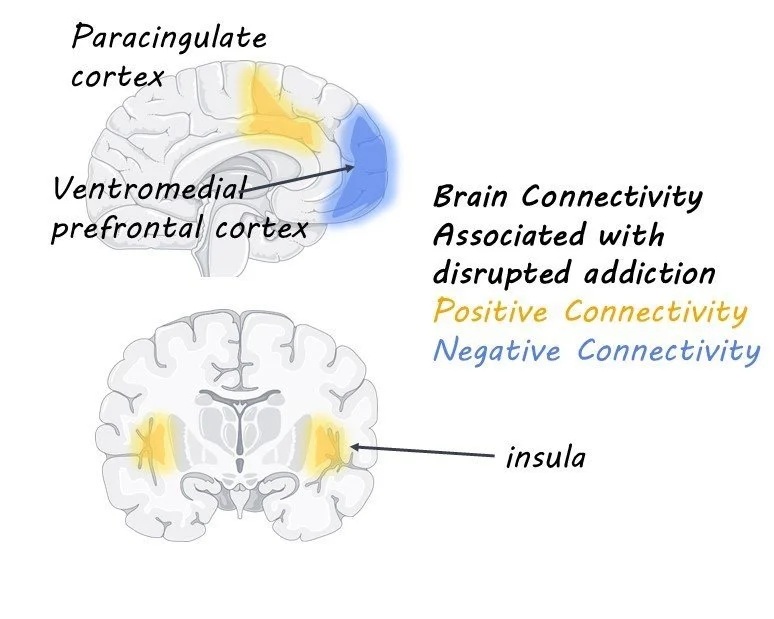
The authors found that lesions that led to a disruption in nicotine addiction occurred in multiple different brain regions. These data suggest that there is no one specific brain region implicated in addiction remission. However, the lesions all had the same pattern of connectivity to brain regions implicated in models of addiction. Brain regions that best matched the connectivity pattern of the lesions included the frontal operculum and paracingulate cortex. This study helps explain why some previous studies found that lesions to the insula are more likely to lead to remission while others have not replicated those results; lesions map to specific brain circuits, not specific regions.
What's the impact?
This study is the first to show that brain lesions that disrupt addiction map to specific brain circuits. This work has therapeutic potential, as neuromodulation techniques such as DBS and TMS may be most effective if they target brain regions with the same connectivity profile as the lesions that disrupted addiction in this study. This study provides targets for therapeutic neuromodulation, which has the potential to induce remission in those with SUDs.